Why in News?
- Evidence highlights systemic delays in emergency cardiac care, with patients reaching treatment centres 5–6 hours post-symptom onset, causing preventable deaths.
- Despite schemes like AB-PMJAY, gaps in infrastructure, affordability, and timely response continue to undermine cardiac survival outcomes.
Relevance
- GS II (Health Governance)
- Public health infrastructure, Ayushman Bharat
- GS III (Social Sector)
- Healthcare access, affordability, human capital
Practice Question
Q1.“Time-sensitive healthcare delivery remains a major challenge in India’s health system.”Examine in the context of emergency cardiac care. (250 words)
Overview
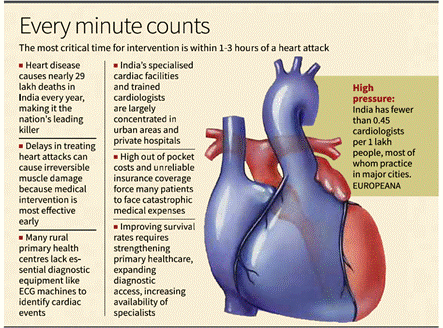
- Cardiovascular diseases cause 28.6 lakh deaths annually, making them India’s leading cause of mortality with earlier onset (45–55 years) than global averages.
- Critical concept: “Time is muscle”—delays in restoring blood flow lead to irreversible cardiac damage and increased mortality risk.
- Global standard: ECG within 10 minutes, angioplasty within 90 minutes (door-to-balloon time); Indian reality averages 300–360 minutes delay, extending to 12 hours in hilly regions.
- Survival exceeds 90% if treated within 1 hour, but every 30-minute delay increases 1-year mortality by 7.5% (Indian Heart Journal, 2025).
- Only 11% patients reach appropriate facility within 1 hour (Faridabad study, 2023) due to lack of awareness, transport, and misdiagnosis at first contact points.
- Rural PHCs often lack ECG machines (<25% functional availability) despite National Essential Diagnostic List mandate.
- India has ~2,500 cath labs, with 70% concentrated in 5 states and ~90% in private sector, creating rural “cardiac care deserts.”
- Severe human resource gap: ~5,500 cardiologists (≈0.45 per 100,000 population), heavily urban-centric, limiting emergency response capacity.
- Patients face high out-of-pocket expenditure (₹1.5–3.5 lakh per procedure); nearly 50% households incur catastrophic health expenditure.
- Despite Ayushman Bharat (AB-PMJAY), reimbursement gaps and private hospital refusal reduce effective financial protection.
Static Background
Cardiac Emergency Care Basics
- Heart attack (Acute Myocardial Infarction) occurs due to blockage of coronary arteries, requiring immediate restoration of blood flow via angioplasty or thrombolysis.
- Key timelines: Golden Hour (first 60 minutes) and 1–3 hour critical window determine survival and long-term cardiac function.
Health System Structure
- Primary Health Centres (PHCs) → first contact, but lack diagnostics.
- Community/District Hospitals → limited specialists and infrastructure.
- Tertiary Hospitals → cath labs and cardiologists, mostly urban/private.
Policy Context
- Ayushman Bharat (PMJAY) aims to provide ₹5 lakh health cover, but implementation gaps persist.
- National Essential Diagnostic List mandates ECG availability at PHC level, yet compliance remains poor.
Key Structural Gaps Identified
- Pre-hospital delay due to low symptom awareness, poor ambulance networks, and geographic barriers in rural/hilly regions.
- Diagnostic gap at PHC level due to absence of ECG machines and trained personnel for interpretation.
- Treatment infrastructure gap with uneven distribution of cath labs and cardiologists across states.
- Underutilisation of thrombolysis due to fear among non-specialist doctors and lack of protocol-based decision systems.
- Financial barriers despite insurance schemes, leading to delayed or forgone treatment.
Innovative Solution: Hub-and-Spoke Model
- Spokes (PHCs/CHCs) equipped with portable ECG devices and trained nurses for first-level diagnosis.
- Hub (district/private hospitals) provides real-time ECG interpretation via telemedicine platforms.
- Enables early thrombolysis (Tenecteplase) at peripheral centres if angioplasty facility is >2 hours away.
- Proven impact: STEMI Karnataka & Tamil Nadu TAEI reduced treatment delays by ~40%, improving survival outcomes.
- Integration with digital platforms and AI-based ECG interpretation enhances scalability and cost-efficiency.
Challenges / Criticisms
- Geographic inequality: Remote and hilly regions face extreme delays due to terrain and poor connectivity.
- Digital divide limits effectiveness of telemedicine-based solutions in low-connectivity regions.
- Human resource shortages in cardiology and emergency care weaken last-mile implementation.
- Insurance inefficiencies: Denial of treatment or informal payments reduce trust in public schemes.
- Protocol gaps: Lack of standardised emergency response systems across states leads to inconsistent care delivery.
- Behavioural barriers: Low awareness and cultural hesitation delay decision to seek immediate care.
Way Forward
- Ensure universal ECG availability at PHC level with AI-enabled interpretation to overcome specialist shortage.
- Scale up hub-and-spoke cardiac networks nationally, integrating telemedicine and emergency transport systems.
- Strengthen ambulance infrastructure (108 services) with GPS tracking and cardiac care protocols.
- Expand public cath lab infrastructure in underserved districts to reduce geographic disparities.
- Reform AB-PMJAY reimbursement rates and enforcement mechanisms to ensure private sector participation.
- Promote mass awareness campaigns on heart attack symptoms and urgency (like “Act FAST” campaigns).
- Integrate cardiac care into Health and Wellness Centres (HWCs) under Ayushman Bharat for preventive and early detection strategies.
Prelims Pointers
- Door-to-balloon time: <90 minutes (global standard).
- Golden hour: first 60 minutes critical for survival.
- India: 28.6 lakh annual CVD deaths.
- ~2,500 cath labs; 90% private sector.
- <25% rural PHCs have ECG facilities.
- 50% households face catastrophic expenditure in cardiac care.



