CONTENTS
- What’s Missing in the Disaster Database?
- The Delicate Balancing of Health-Care Costs
What’s Missing in the Disaster Database?
Context:
In 2023, the Food and Agriculture Organization of the United Nations highlighted that global disaster events have surged from 100 per year in the 1970s to around 400 per year in the last two decades. However, an analysis of disaster databases reveals that this increase is partly due to reporting bias. While data from various disaster events helps identify patterns in factors like increased resilience, climate change, and humanitarian response, smaller events with less damage or fatalities are often absent from historical records.
Relevance:
GS3- Disaster Management
Mains Question:
Do disaster databases in India suffer from a reporting bias? What can be done to promote better reporting of disasters in India? (10 Marks, 150 Words).
Relevant Statistics:
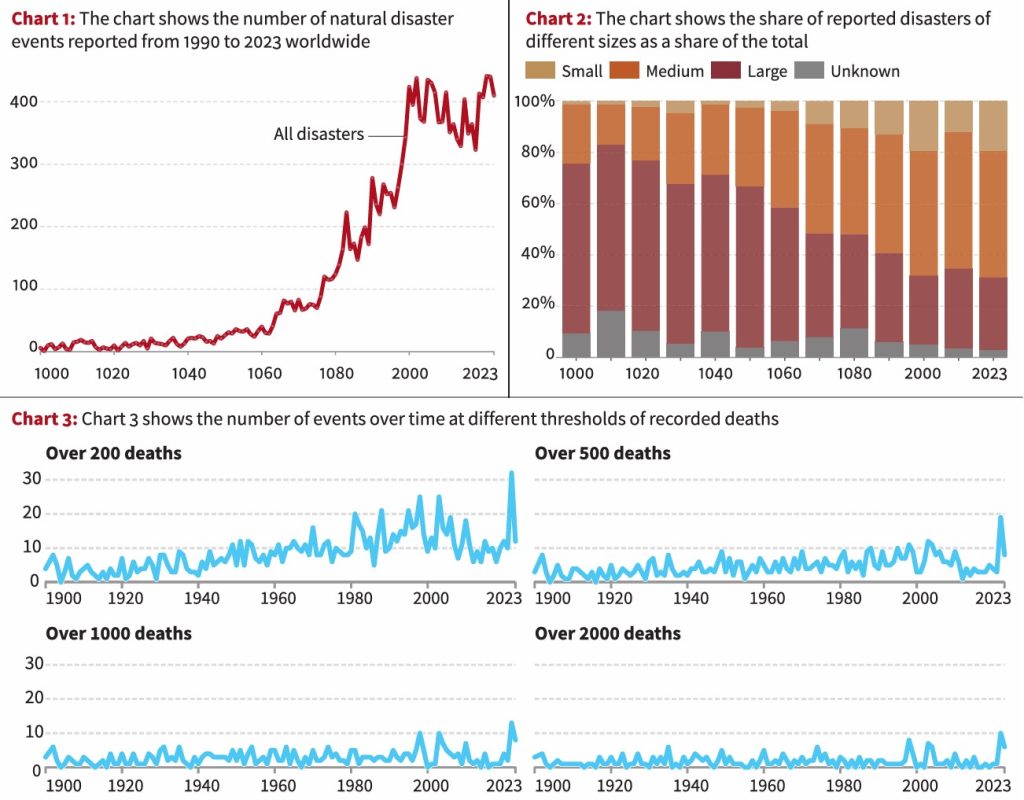
- Chart 1 illustrates the number of reported natural disaster events worldwide from 1990 to 2023. Recently, the reporting and communication of smaller events have improved.
- In a 2004 report, CRED noted that historical data was based on retrospective analysis, mainly listing events of major significance.
- This was due to the underdevelopment of humanitarian aid and telecommunications, and the lack of interest from organizations in compiling data on natural disasters.
- Chart 2 shows the proportion of reported disasters of different sizes as a share of the total. As we look further back in time, large events increasingly dominate the records. Small and medium events were often missed at the time and are now impossible to identify.
- The trend for small events, with fewer than 200 deaths, rose significantly in the 1980s and 1990s, indicating that small events were underreported in earlier periods and have only been consistently reported in the past 30 to 40 years.
- Chart 3 illustrates the number of events over time at different thresholds of recorded deaths, showing that the patterns observed are largely due to progressively better reporting of natural disaster events worldwide.
Gaps and Inconsistencies Revealed:
- Disaster data also reveal significant gaps, particularly in economic damages. More than 40% of disasters between 1990 and 2020 did not have estimated monetary damages.
- The data on insured damages were even more incomplete, missing 88% of the time, while 96% had no records of reconstruction costs.
- Data coverage tends to be poorer in low-income countries. For example, from 2000 to 2019, only 13% of disasters in Africa and 23% in South Asia reported any economic losses.
- Disaster statistics also reveal inconsistencies for different types of disasters.
- Firstly, many regions, such as Sub-Saharan Africa, have poor data coverage and are often completely overlooked.
- Secondly, over half of the reported heat events came from just a few countries: Japan, India, Pakistan, the U.S., France, Belgium, the U.K., Spain, and Germany.
- It is unlikely that these are the only countries experiencing extreme heat events; rather, these events are not being recorded or estimated in other regions.
- Additionally, accurately quantifying the health effects of extreme temperatures is challenging. Most heat-related deaths result from an increased risk of less obvious conditions, such as cardiovascular disease.
- These indirect deaths are not noted as “heat-related” at the time and can only be estimated later using statistical methods.
- This applies to both heat- and cold-related deaths, which are likely underreported due to reporting biases, leading to significant inequalities.
Conclusion:
Disasters often have immediate and acute impacts on human mortality, health, and infrastructure. However, disasters like droughts can also lead to indirect, medium-to-long-term impacts, such as malnutrition and food insecurity, which are harder to quantify. Improper reporting of disasters can lead to insufficient efforts towards disaster mitigation.
The Delicate Balancing of Health-Care Costs
Context:
As we navigate the evolving landscape of Indian healthcare, cost considerations are increasingly influencing every aspect of service delivery and patient care. With growing health disparities and uneven access to medical services, the need for equitable and sustainable healthcare policies is more urgent than ever.
Relevance:
GS2-
- Health
- Government Policies & Interventions
GS3-
- Government Budgeting
- Planning
Mains Question:
Access, innovation, and affordability need to be kept in mind while shaping equitable and sustainable health-care policies. Analyse. (10 Marks, 150 Words).
Setting Rates for Medical Services:
- Ongoing discussions about setting rates for medical services are not mere bureaucratic exercises; they fundamentally shape how we perceive, access, and deliver healthcare across India.
- In this globalized era, responses to similar challenges worldwide vary, influenced by different cultural, economic, and systemic factors.
- By learning from these international examples, we can refine our strategies to manage healthcare costs more effectively.
- Private hospitals are not only centers of specialized care but also hubs of innovation. Consider the Joint Commission International (JCI) and National Accreditation Board for Hospitals (NABH)-accredited major hospital groups, which have embraced cutting-edge technologies to significantly enhance patient outcomes, particularly in complex procedures.
- These institutions invest heavily in top-tier infrastructure and advanced technologies, enabling them to seamlessly integrate telemedicine and remote care, thus broadening access and building patient trust.
Price Caps, Quality and Innovation:
- As the Supreme Court considers standardizing medical procedure rates across both government and private sectors, affordability becomes a key focus. However, imposing uniform price caps might significantly compromise healthcare quality.
- According to a Health Care Management Review study, hospitals facing financial pressure from price caps report a 15% increase in patient dissatisfaction.
- Additionally, such caps could slow the development of new treatments and technologies, especially in areas like cancer research and robotic surgery, where substantial investment is essential.
- Could value-based pricing, which ties payments to health outcomes rather than service volume, be a viable solution?
- The broader economic impacts of healthcare pricing policies extend beyond the healthcare sector itself.
- While properly implemented rate standardization can help reduce healthcare disparities, we must ensure it doesn’t destabilize providers’ financial stability.
- Economists suggest dynamic pricing models that adjust based on medical complexity and patients’ financial status, providing a fair solution.
- For example, Thailand’s tiered pricing system, which considers patient income levels and medical necessity, effectively balances cost and care and could serve as a model for India’s diverse economic landscape.
Legal and Regulatory Challenges:
- Effectively managing healthcare costs requires legislative reform. Tailoring approaches to accommodate local demographic and economic conditions can support rate standardization and ensure high-quality care.
- States like Rajasthan and Tamil Nadu have identified gaps in rate fixation provisions and advocate for robust legal frameworks to address these issues.
- Technology is revolutionizing healthcare by making diagnostics faster and more accurate with artificial intelligence and improving care coordination through electronic health records.
- For instance, telemedicine initiatives in Karnataka have reduced hospital visits by 40%, demonstrating how technology can make medical care more accessible and cost-effective, especially in remote areas.
- This integration reduces pressure on healthcare facilities while providing timely care directly to patients’ homes.
- Additionally, innovations such as mobile health apps and wearable devices are crucial for managing chronic conditions outside hospitals, significantly cutting costs and enhancing patient outcomes. Ensuring that these technologies reach all population segments is essential.
- Investing in infrastructure for broader Internet access and improving digital literacy will enable more people to benefit from these advancements, positioning India as a global leader in healthcare innovation.
- Recent surveys of healthcare professionals across India highlight a consensus on the need for flexible pricing strategies that reflect the complexities of medical procedures and patient-care requirements.
- Engaging all stakeholders, including private healthcare providers, is essential to understand the nuanced dynamics and develop effective, sustainable policies.
Role of Data in Shaping Policies:
- In the era of big data, healthcare policy decisions should increasingly be based on data-driven insights.
- Data analytics can illuminate patient outcomes, treatment efficacy, and cost efficiency, informing more nuanced rate-setting frameworks.
- Additionally, predictive analytics can forecast the long-term impacts of rate fixation on healthcare innovations, enabling policymakers to adjust regulations to foster both innovation and accessibility.
- Balancing access, innovation, and affordability in healthcare is delicate but essential. Implementing pilot projects in select districts can help gauge the impact of rate caps on healthcare quality and innovation.
- Allocating government subsidies to support research and development in private hospitals and establishing public-private partnerships to integrate cutting-edge technologies in public hospitals are also recommended. These measures can ensure widespread access to advanced healthcare solutions.
Conclusion:
As India aims to become a global healthcare leader, it is crucial to foster an environment that encourages innovation while ensuring equitable access to quality healthcare. Prioritizing the well-being of every individual is essential, as emphasized by a member of the NITI Aayog: “Affordable healthcare is not just a necessity but a priority for our nation, and we are committed to innovating and leveraging technology to bring down healthcare costs for every citizen.”



